Breast reconstruction in obese patients: challenges and strategies
Authors:
Alessia M. Lardi1,2,4
Martina Maranta3
Doris Babst2
Hanna V. Riedmann1
Pia Wittlin1
1 Department for Plastic, Reconstructive, and Aesthetic Surgery, Cantonal Hospital Graubünden
2 Centre for Plastic Surgery, Dr. Babst, Bern
3 Department for Gynaecology, Cantonal Hospital Graubünden
4 Clinic Beethovenstrasse, Zurich
Correspondence:
E-Mail: alessia.lardi@ksgr.ch
Sie sind bereits registriert?
Loggen Sie sich mit Ihrem Universimed-Benutzerkonto ein:
Sie sind noch nicht registriert?
Registrieren Sie sich jetzt kostenlos auf universimed.com und erhalten Sie Zugang zu allen Artikeln, bewerten Sie Inhalte und speichern Sie interessante Beiträge in Ihrem persönlichen Bereich
zum späteren Lesen. Ihre Registrierung ist für alle Unversimed-Portale gültig. (inkl. allgemeineplus.at & med-Diplom.at)
Obesity has emerged as one of the most prevalent chronic diseases in Europe and represents a major challenge for contemporary surgical care. Defined by the World Health Organization (WHO) as a body mass index (BMI) ≥30kg/m² and categorised into three severity classes, its prevalence has increased dramatically – by 138% in Europe between 1975 and 2016. Today, more than half of European adults are overweight or obese.¹,² In Switzerland in 2022, 31% of adults were overweight and 12% obese, with further increases expected in the coming decades.³
For surgery and peri-operative management, this demographic shift is highly relevant. Obesity frequently coexists with metabolic and cardiopulmonary comorbidities—including diabetes mellitus, arterial hypertension, cardiovascular disease, cerebrovascular events and venous thromboembolism—that collectively heighten the peri-operative risk.4 Excess subcutaneous adiposity further complicates surgical exposure and increases technical demands, resulting in prolonged operative time.5
As breast reconstruction is increasingly performed in this population, a clear understanding of how obesity alters risk profiles and surgical decision-making becomes essential. The following sections therefore outline the considerations by which obesity shapes postoperative outcomes and discuss how these considerations should influence the selection and execution of reconstructive strategies.
Obesity in reconstructive breast surgery
Obesity affects postoperative outcomes through a combination of systemic comorbidities, altered tissue biology and mechanical factors; peri-operative morbidity across surgical specialties is amplified.5 These systemic risks intersect with local tissue vulnerabilities: increased adipose content is associated with reduced perfusion, impaired oxygenation and diminished microvascular reserve, all of which predispose to delayed wound healing, infection and fat necrosis.7,8 Adipose-rich tissues also tend to create larger potential dead spaces, contributing to higher seroma rates.6,8 In the context of autologous tissue microsurgical transfer, these biological limitations may translate into higher rates of vascular complications—including arterial thrombosis and flap loss—particularly when flap weight increases pedicle strain or exceeds the capacity of the available blood supply.9,10 Medical complications such as deep vein thrombosis and pulmonary embolism are likewise more common in obese patients and contribute substantially to postoperative morbidity.4
Breast-conserving therapy
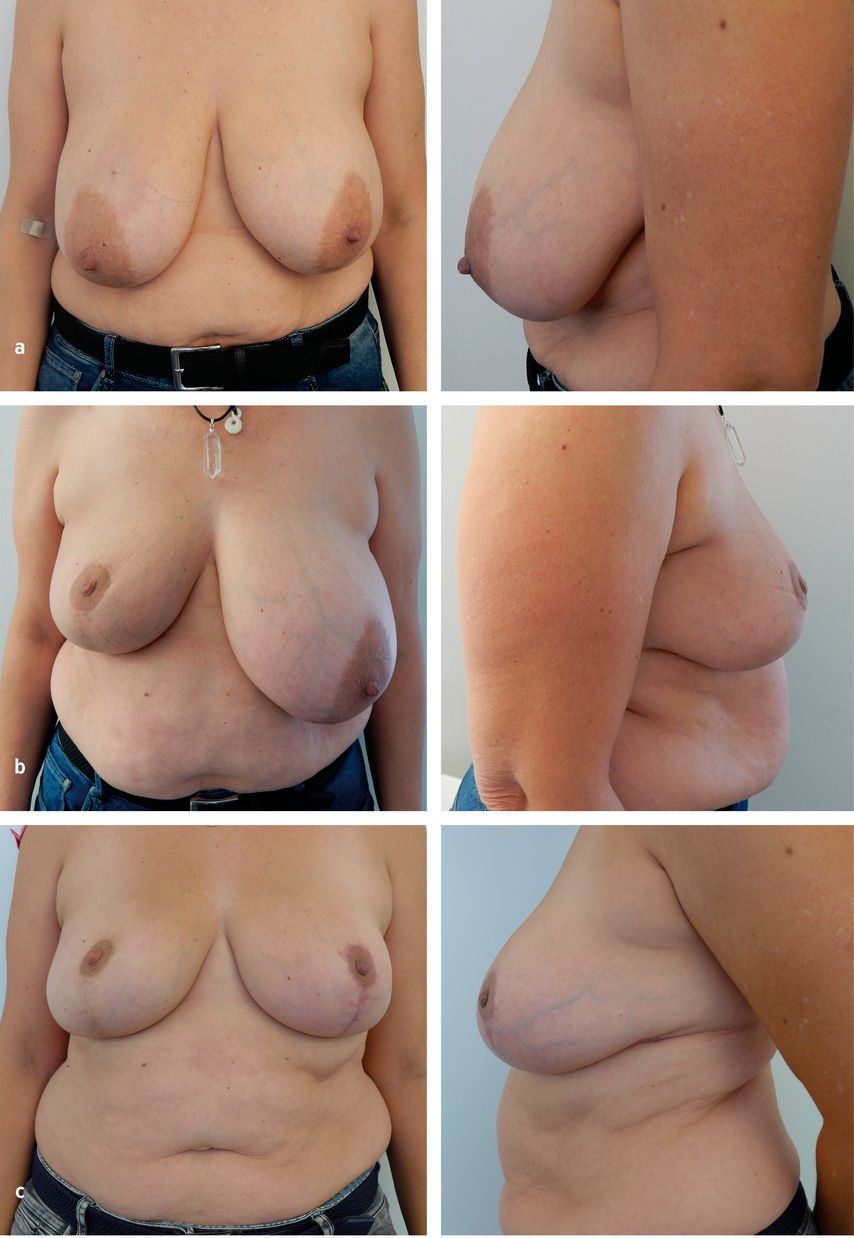
Understanding these mechanisms is essential for tailoring reconstructive planning. Procedure selection, flap design, device-fill strategy, staging and perfusion assessment must all account for the altered risk landscape inherent to obesity principles that inform the reconstructive strategies detailed in the subsequent sections. For many women with overweight or obesity, breast-conserving therapy (BCT) is not only feasible but often advantageous precisely because of breast size. Larger native volume provides generous oncoplastic reconstructive options. In the first step, the cancer-side operation combines a wide local excision with a tailored oncoplastic reconstruction. Once adjuvant therapy is complete and tissues have settled, a second-stage contralateral symmetrisation refines balance and addresses any radiotherapy-related asymmetry (Fig. 1). Complication risks in women with obesity are dehiscence at T-points, fat necrosis and delayed healing. In obese patients rates are higher than in leaner cohorts, yet remain acceptable with careful design, preservation of perfusion, discreet resection weights and meticulous closure. Contemporary data are reassuring that standardised pathways allow adjuvant therapy to proceed on schedule even in higher-BMI groups.11
Fig. 1: 48-year-old woman, BMI 31 kg/m² — right breast cancer treated with segmentectomy and oncoplastic reconstruction. a) Pre-operative baseline. b) Early post-op after right segmentectomy + oncoplastic reconstruction. c) Long-term result after adjuvant chemotherapy and radiotherapy (total 50.05 Gy) and contralateral left reduction mastopexy
Alongside oncoplastic techniques, perforator-based volume replacement flaps expand the reconstructive options in this cohort. The thoracodorsal artery perforator flap (TDAP/T-DAP) and the lateral intercostal artery perforator flap (LICAP) are particularly useful when resection would otherwise jeopardise contour or when tumour location limits classical oncoplastic reconstructions. Both flaps are pedicled, muscle-sparing and draw upon tissue that is frequently abundant in women with higher BMI. Lateral thoracic and axillary fullness for the LICAP, and the latissimus territory for the TDAP allow reliable replacement of a substantial segmental deficit without the donor-site morbidity of a muscle harvest. In the lateral and lower-outer quadrants, a LICAP can be designed along the posterior axillary line or lateral inframammary fold. When additional reach or bulk is required, the TDAP offers a longer arc of rotation with supple tissue that tolerates postoperative radiotherapy.12,13
Selecting BCT in this population should be led by morphology as much as BMI. Large, ptotic breasts with a favourable tumour-to-breast volume ratio are ideal. Multifocality, inflammatory disease and unfavourable tumour–breast relationships may still indicate mastectomy. Where mastectomy is chosen for morphology rather than mandate, skin-reducing mastectomy (SRM) offers a controlled reconstructive platform.19,20
Implant-based reconstruction
Implant-based reconstruction is still the most common used approach. Operating time is shorter and physiological stress lower, which explains its popularity in higher-BMI cohorts. The trade-off is a higher risk of seroma, infection and device loss, with five-year loss rates approaching one in six in women with obesity compared with roughly one in fourteen in women of normal weight.14–16 Risks are modulated by plane of placement, soft-tissue support and fill strategy. Pre-pectoral devices avoid animation but set a higher risk for flap quality. Subpectoral pockets or staged expanders remain well-considered when perfusion is borderline. Liberal use of acellular matrices in adipose envelopes invites seroma and potentially infections, whereas an SRM-derived inferior dermal sling can provide vascularised internal support and reduce foreign material.21–23
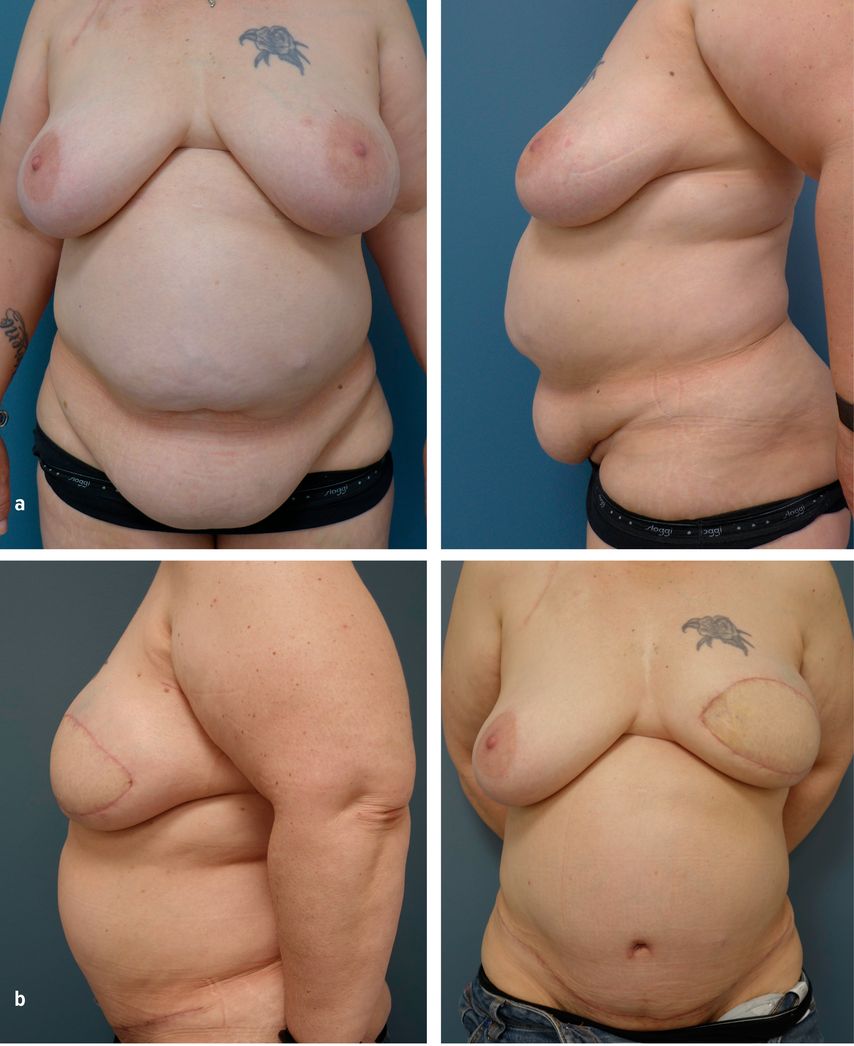
By contrast, autologous reconstruction—most commonly a DIEP flap—tends to deliver more stable long-term shape and higher patient-reported satisfaction than implants, including higher-BMI cohorts (Fig.2).17,18
Fig. 2: 50-year-old woman, BMI 39 kg/m² — left modified SSM (due to inflammatory breast cancer) with immediate DIEP reconstruction after neoadjuvant treatment; adjuvant radiotherapy total dose 52.5 Gy. a) Pre-operative baseline following neoadjuvant treatment. b) Early post-operative appearance after left skin-sparing mastectomy and immediate DIEP flap reconstruction
The principal medical risk is venous thromboembolism, which rises with BMI and operative time and must be met with personalised thromboprophylaxis and early mobilisation.4 The main technical pitfalls in this group are mechanical—weight, depth of operation site and perfusion—and they are solvable with deliberate technique. Flap harvesting and handling are more demanding because adipose flaps are heavier and less forgiving of torsion. Dissection must be deliberately atraumatic, with broad-based handling and no point-loading of the pedicle. Instruments and assistants should be arranged so that the flap is supported throughout inset, not suspended from a single corner.
Perfusion deserves objective measurement: in higher-BMI flaps, a single perforator that would work out in a leaner patient may be inadequate. It is well-considered to identify and preserve a second perforator where anatomy allows, or to choose a dominant perforator with high calibre and short intramuscular course. Indocyanine-green angiography pragmatically confirms arterial inflow and guides conservative peripheral trimming to reduce fat necrosis.19 Microsurgical exposure can be constrained by thicker subcutaneous layers and shorter working distances, therefore, creating a clean, shallow tunnel to the recipient site before bringing the flap into the field preserves space. Where recipient vessels are tight in a deep chest wall, a modest extension of the incision for direct, non-angulated work is safer than an anastomosis at depth. Fixation must assume that the flap is heavy on day one and heavier after oedema peaks. This is why suturing to load-bearing points—pectoral fascia or robust dermis—ensures the pedicle carries no weight. Donor-site closure under tension is unforgiving in thick abdominal walls so that progressive-tension sutures and closed incision negative pressure dressings may reduce seroma and dehiscence.
Conclusion
Obesity is one of the defining challenges of nowadays in breast reconstruction. Excellent results now depend not only on operative precision but on individualised planning, explicit risk stratification and strong multidisciplinary collaboration. A morphology-led pathway that moves from BCT and perforator solutions on to implant or autologous reconstruction as indicated enables safe and durable results in women with overweight and obesity. Implants remain useful but attract more complications, whereas autologous options offer superior long-term quality of life when the technical and thromboembolic challenges are addressed directly.
Literatur:
1WHO: Obesity and overweight. Fact sheet (accessed 12.11.2025)2 NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in BMI 1975–2016. Lancet 2017; 390: 2627-42 3 Bundesamt für Statistik (BFS): Übergewicht/Adipositas Schweiz 2022 (accessed 12.11.2025) 4 Ageno W et al.: Cardiovascular risk factors and venous thromboembolism: a meta-analysis. Circulation 2008; 117: 93-102 5 Ri M et al.: Obesity as a surgical risk factor. Ann Gastroenterol Surg 2018; 2: 13-21 6 McCarthy CM et al.: Predicting complications after expander/implant breast reconstruction. Plast Reconstr Surg 2008; 121: 1886-92 7 Pierpont YN et al.: Obesity and surgical wound healing: a current review. ISRN Obes 2014; 2014: 638936 8 Wilson JA, Clark JJ: Obesity: impediment to wound healing. Crit Care Nurs Q 2003; 26: 119-32 9 Fischer JP al.: Free tissue transfer in the obese patient: outcomes and cost in 1,258 abdominally based reconstructions. Plast Reconstr Surg 2013; 131: 681e-92e 10 Chang DW et al.: Effect of obesity on flap and donor-site complications in TRAM breast reconstruction. Plast Reconstr Surg 2000; 105: 1640-8 11 Fortenbery L et al.: Oncoplastic reduction mammoplasty in high-BMI patients: complications and adjuvant timing. PRS Global Open 2024; 12: e5600 12 Hamdi M et al.: Pedicled perforator flaps in breast reconstruction: a new concept. Br J Plast Surg 2004; 57(6): 531-9 13 Hamdi M et al.: The lateral intercostal artery perforators: anatomical study and clinical application in breast surgery. Plast Reconstr Surg 2008; 121(2): 389-96 14 ElAbd R et al.: Autologous versus alloplastic breast reconstruction in obese patients: systematic review and meta analysis. Aesthetic Plast Surg 2022; 46(2): 597-609 15 Leitner L et al.: Outcomes after implant-based breast reconstruction: 17-year single-centre experience. J Clin Med 2021; 10(23): 5665 16 Vaccari S et al.: Implant-Based Breast Reconstruction: Impact of Body Mass Index on Postoperative Complications and Aesthetic Results: A 5-Year, Single-Center Study. Aesthet Surg J 2023; 43(12): NP1063-NP1070 17 Srinivasa DR et al.: Direct-to-Implant versus Two-Stage Tissue Expander/Implant Reconstruction: 2-Year Risks and Patient-Reported Outcomes from a Prospective, Multicenter Study. Plast Reconstr Surg 2017; 140(5): 869-77 18 Frid M et al.: A systematic review on the association between body mass index and autologous breast reconstruction. Ann Breast Surg 2024; 8: 18 19 Robertson SA et al.: Mastectomy skin-flap necrosis: challenges and solutions. Breast Cancer (Dove Med Press) 2017; 9: 141-52 20 Cheong SC et al.: Wise versus vertical mastopexy pattern SRM: comparative analysis. Plast Reconstr Surg Glob Open 2025; 13(3): e6584 21 Korwar V et al.: Skin-reducing mastectomy with immediate reconstruction using an inferior dermal sling. Am J Surg 2014; 208: 240-8 22 Jepsen C et al.: Complications, patient-reported outcomes, and aesthetic results in immediate breast reconstruction with a dermal sling: A systematic review and meta-analysis . J Plast Reconstr Aesthet Surg 2019; 72(3): 369-80 23 Lo Torto F et al.: Patient-selection score (including SSM/NSM) to guide pre-pectoral reconstruction. J Clin Med 2024; 13: 6466
Das könnte Sie auch interessieren:
Schwangerenvorsorge in Deutschland
Die Schwangerenvorsorge begleitet werdende Mütter vom Beginn der Schwangerschaft bis zur Geburt. Sie dient der frühzeitigen Erkennung von Risiken, der Überwachung der kindlichen ...
Diagnostik und Therapie des Zervixkarzinoms
Weltweit werden jährlich über 500000 neue Zervixkarzinome diagnostiziert, überwiegend in ressourcenarmen Regionen. Dagegen sind Zervixkarzinome in entwickelten Ländern extrem selten ...
Diagnostik, Überwachung und Therapie bei Präeklampsie
Die Präeklampsie (PE) ist mit einem hohen Risiko für maternale und fetale Komplikationen verbunden und erhöht zugleich das langfristige kardiovaskuläre Risiko betroffener Frauen. Eine ...